What is type 2 diabetes?
More than 200,000 people are diagnosed with type 2 diabetes every year. Diabetes increases the risk of serious health complications and early death. Modern life can make it hard to be healthy, but for many people type 2 diabetes can be prevented by making small lifestyle changes. Diabetes is a leading cause of vision loss and blindness in people of working age. People with diabetes are up to five times more likely to develop heart disease or have a stroke than those without diabetes. However, Type 2 diabetes can be prevented by:
• managing your weight
• eating healthily
• being more active
Making small changes to your lifestyle now can make a big impact on your future health and having experts to help you make the right choices along the way can make it even easier.
 Where else can I find helpful information?
Where else can I find helpful information?
Some useful websites:
NHS Diabetes Prevention Programme
What are the signs and symptoms of type 2 diabetes?
When you have type 2 diabetes your body cannot get enough glucose into your cells, so a common symptom is feeling very tired. There are also other symptoms to look out for. These include feeling thirsty, going to the toilet a lot and losing weight without trying to.
The symptoms of type 2 diabetes can develop more slowly than the symptoms of type 1 diabetes, making the condition harder to spot. That’s why a lot of people don’t get any symptoms or don’t notice them.
Some people also do not think the symptoms are important, so do not ask for help. This means some people can live for up to 10 years with type 2 diabetes before being diagnosed.
Risk of cardiovascular disease (CVD) in patients with diabetes
When you have diabetes, you're more at risk of heart disease. This is also called cardiovascular disease (CVD) or coronary disease, and can lead to heart attacks and strokes. Cardiovascular disease affects your circulation too. And poor circulation makes other diabetes complications worse – like problems with your eyes and feet. That’s why it’s even more important to take good care of your heart when you have diabetes.
If you have high blood sugar levels for a period of time, even slightly high, your blood vessels can start to get damaged and this can lead to serious heart complications. This is because your body can't use all of this sugar properly, so more of it sticks to your red blood cells and builds up in your blood. This build-up can block and damage the vessels carrying blood to and from your heart, starving the heart of oxygen and nutrients. Even mildly raised blood sugar levels can, over time, put you more at risk.
What are SGLT2 inhibitors?
SGLT2 inhibitors are a type of oral medication used to treat type 2 diabetes. They are also called sodium-glucose co-transporter-2 inhibitors (SLGT2i) or gliflozins. SGLT2 inhibitors are tablets that can help to lower your blood glucose (sugar) levels. If you have type 2 diabetes, your doctor may prescribe them as part of your treatment plan.
SGLT2 inhibitors can help to lower your blood sugar levels by:
- reducing the amount of glucose being absorbed in the kidneys so that it is passed out in the urine
- reducing the amount of glucose in your blood.
How well they work will depend on your kidney function. If you take SLGT2 tablets, you may experience some side effects. Check the Patient Information Leaflet (PIL) that comes with your medication. If you think you may be experiencing any of the side effects, speak to your GP straight away. It’s also important to be aware that your urine will test positive for glucose if you take this medication.
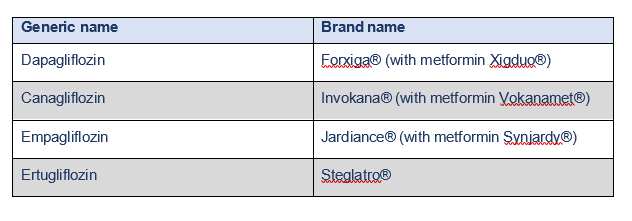
There are several different tablets in the SGLT2 group.
Further information on Dapagliflozin and Empagliflozin
Who can use SGLT2 inhibitors
SGLT2 inhibitors may be suitable for people with type 2 diabetes that have high blood glucose levels despite being on a medication regimen such as metformin and insulin.
SGLT2 inhibitors are not recommended to people with kidney disease as this condition prevents the drug from working sufficiently well.
SGLT2 inhibitors can:
- help to reduce the risk of cardiovascular disease
- aid weight loss
- help to remove glucose from the blood and lower blood glucose levels
Side effects of SGLT2 inhibitors
As with every medication, also SGLT2 inhibitors may have some side effects. Your doctor will ensure this medication is suitable for you.
As the drugs cause more glucose to be excreted in the urine, there is a higher chance of getting genital and urinary tract infections. These side effects are more common in women than in men.
Taking SLGT2 inhibitors with insulin, sulphonylureas or glinides may increase the risk of hypoglycemia. SGLT2 inhibitors can, in rare cases, lead to a dangerous condition called diabetic ketoacidosis.
It is ok to ask questions about your medication
So that you can get the best out of your medication, it is important that you ask your GP or any healthcare staff at your surgery any question that can help you understand:
- why you have been prescribed a medicine
- what its benefits are
- what its side effects are
- any interactions with other medications
Everyone should be able to ask about their medicines
‘Me and My Medicines’ is a campaign led by patients and supported by clinical staff to help people raise concerns and use their medicines better. This will help everyone benefit from more effective and safer care. You can find out more about this campaign on the 'Me and My Medicine' website
New Medicine Service
The New Medicine Service is a free NHS consultation, offered through your pharmacy, to help you understand your condition, get the most out of your new medicine(s) and discuss any concerns. The pharmacist will:
- help you to find out more about the new medicine(s) you are taking
- help to sort out any issues you are having with your new medicine(s)
- give you a chance to ask questions about your medicine(s) and discuss any concerns
- help to improve the effectiveness of your new medicine, for example, there may be an easier or better way to take it
- help you to make your own decisions about managing your condition
- help you to improve your health, which could lead to fewer GP and hospital visits
Ask your GP or local pharmacy to learn more about this service.